Training the next generationof musculoskeletal interface scientists
We aim to unravel MSK interface structure–function relationships from the macro- to molecular scale, addressing fundamental questions in:
- Bone–tendon and muscle–tendon interfaces
- Bone quality and mineral–collagen interactions
- Osteocyte lacunar-canalicular networks & mechanobiology
- Age-, sex- and gender-specific differences in MSK health
- Regeneration and remodeling in zebrafish and mammalian models
- AI-enhanced image analysis
- Computational modeling of interfaces
Our projects address these by integrating different approaches, ranging from synchrotron imaging, ultra-high-resolution electron microscopy (TEM, SBF-SEM, FIB-SEM), nano- and micro-CT, SAXS/WAXS, Raman spectroscopy, optical coherence tomography, advanced biomechanics, Finite-Element-Methods & Finite Cell Methods to AI-driven analytics into unified, correlative workflows.
P1
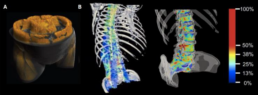
Assessing the impact and predictive value of bone marrow fat, BMD, muscle mass, and muscle fat on fracture risk and outcome using spectral-CT imaging
Main supervisor: Isabel Molwitz (UKE)
Co-Supervisors: Tobias Knopp (TUHH/UKE) & Alexander Schlaefer (TUHH)
Research background and question
Muscle quality has recently gained interest as a potentially superior, predictive imaging biomarker for, e.g., survival, compared to muscle mass [3-5]. CT allows to quantify bone and muscle mass. Muscle quality used to be assessed indirectly by CT density reflecting myosteatosis. CT density, however, is affected by contrast agents. Spectral CT scanners now enable non-invasive quantification of bone and muscle fat, and BMD unbiased by contrast agent [1,2,7]. Pioneering work on the predictive value of spectral CT muscle fat quantification, demonstrated superior impact of quantified muscle fat over muscle density or muscle mass, as conventional sarcopenia criterion, for mortality and morbidity in critically ill patients [6]. This project will extend the approach of utilizing quantification parameters readily available from clinical routine spectral CT scans with a first investigation of the predictive value of bone marrow fat and the combination of bone and muscle quality parameters for fracture risk, adverse outcome, and survival. Also, it will serve to implement enhanced AI-based image analysis to increase predictive value and clinical applicability further.
Specific aims
- Determine the predictive value of bone marrow fat quantified using spectral-CT techniques with enhanced AI-based image analysis for fracture risk, adverse outcome, and survival.
- Evaluate the complex interaction of bone, muscle, and fat contents for a more precise prediction of fracture risks, adverse outcomes, and reduced survival.
Work program and methods
In this project, the student will perform spectral-CT material quantification for soft tissue, fat, and bone mineral in retrospectively available clinical image datasets. The focus will be on older patients (>60 years; sample size testing: n=762) who received CT scans including the column vertebrae, e.g., exams of the aorta. Data on adverse outcomes such as hospitalizations, surgery, and survival will be derived from electronic patient files. Fractures will be detected on initial CT scans and if available follow-up examinations. Deep-learning AI-based tools for 3D segmentation and radiomics for pattern analysis for the muscle will be available from an ongoing DFG-funded project of the supervisor. With the co-supervisors the student will learn to develop similar algorithms for the vertebral bone. The dataset will then be analyzed for 3D BMD, muscle mass, and bone and muscle fat content, including radiomics. This will allow for the evaluation of the predictive value of each component, the selection of leading components, and the creation of a superior prediction model for fracture risk and adverse outcomes.
P2
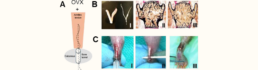
Exploring molecular pathways of tendon-to-bone healing in normal and osteoporotic bone remodeling
Main Supervisor: Johannes Keller (UKE)
Co-Supervisors: Kartharina Jähn-Rickert (UKE) & Sara Checa (TUHH)
Research background and question
Rotator cuff (RC) injuries are among the most common shoulder injuries, especially in older patients with osteoporosis [1], where bone resorption exceeds bone formation. Although there have been significant advances in surgical techniques, there is still a high incidence of RC re-rupture following reconstruction [2,3]. A common site of RC re-rupture is the enthesis. Numerous studies have been conducted to improve tendon integration, but these have primarily focused on the pathophysiological processes within the affected tendon [4]. In contrast, the influence of bone status and local remodeling processes at the bony insertion site on healing outcomes is poorly understood. This is surprising, because tendon is a bradytrophic tissue and adequate healing of tendon into bone is thought to depend primarily on bone processes, including dynamic changes in bone formation by osteoblasts and bone resorption by osteoclasts.
Specific aims
- Multiscale characterization of the impact of osteoporotic bone remodeling on tendon-to-bone and tendon-to-tendon healing (experimental).
- Explore the structure and cellular composition of the tendon-bone interface in patients with RC rerupture (clinical).
Work program and methods
The experimental section relies on the murine Achilles tenodesis model which has significant advantages over other tenodesis (e.g., EC reconstruction) models, including high reproducibility, practicality and the provision of clinically relevant outcome measures. Tendon-bone healing will be characterized in 12–14-week-old WT mice with/without OVX at defined time points. μCT-scanning (osseous changes), histology (structural and cellular histomorphometry), spatiotemporal ultrastructural analysis (mineralization in tendon-to-bone transition, organization of linking collagen fibers at the interface) and biomechanical evaluation of failure force of the evolving tendon-bone interface, will be performed. A cohort in which the Achilles tendon is dissected and reconstructed in the middle (established) will serve as control to differentiate osseous regenerative processes from tendon-to-tendon healing. The clinical section of this project aims to confirm the findings obtained in the mouse model in surgical specimens obtained during revision surgery for reruptured RC tenodesis (supraspinatus). During RC revision surgery, the bone at the previous supraspinatus tendon insertion site is refreshed to cause bleeding, which facilitates tendon-to bone healing. The removed bone including the attached remnants of the ruptured tendon will be used for subsequent multimodal analysis as described above.
P3
The influence of age-related changes in human tendon enthesis, cortical bone microstructure, and myotendinous junction on fracture risk

Main Supervisor: Benjamin Ondruschka (UKE)
Co-Supervisors: Alexander Schlaefer (TUHH) & Sara Checa (TUHH)
Research background and question
Tendon-bone interfaces become increasingly vulnerable to age-related degeneration. Older adults are particularly at risk for tendon disorders and enthesis-related pathologies, which contribute to reduced mobility, chronic pain, and heightened fracture susceptibility. Conditions affecting tendon integrity often lead to functional impairment and the need for surgical intervention [1]. In patients with osteoporosis, tendon detachment and enthesis failure are further aggravated by bone fragility and altered remodeling, increasing the risk of severe injuries such as humeral or femoral fractures following falls. In addition to the hard-soft tissue enthesis interface, the soft-soft tissue myotendinous junction (MTJ) interface is a location where many injuries occur. Yet, the knowledge about its structure and adaptive capacity to training and inactivity is sparse [2]. By investigating how aging and physical activity impacts the integrity and mechanical functionality of tendon interfaces, this research aims to provide a deeper understanding of the mechanisms that contribute to tendon failure and age-related contributors to musculoskeletal fragility.
Specific aims
- Characterize age-related structural and cellular changes in the human tendon enthesis and cortical bone across different age groups using correlative tissue analysis, histology, and immunohistochemistry.
- Assess the biomechanical properties of aging tendons and entheses through tensile testing.
- Investigate the relationship between tendon, cortical bone and MTJ deterioration and its impact on mechanical loading, force transmission, and fracture susceptibility.
Work program and methods
This project will investigate the tendon enthesis, cortical bone microstructure, as well as myotendinous junction to correlate structural alterations at tissue interfaces with biomechanical function and fracture susceptibility. The human cadaveric cohorts will first be categorized into different age groups and scanned using DEXA and CT to extract information on the skeletal status. Post-mortem bone-tendon-muscle samples will be collected through forensic medical investigations. Specimens will include the minor trochanter of the femur and the attached psoas major, selected due to its critical role in locomotion, its exposure to varying mechanical demands, and its known adaptive responses to physical strain. Biomechanical uniaxial tensile testing will be conducted to assess tensile strength, stiffness, and load-bearing capacity of tendon-bone and muscle-tendon specimens according to standardized test protocols [3]. Digital image correlation and stress-strain mapping will provide strain distribution data, allowing for a precise evaluation of mechanical failure points. Histological staining and immunohistochemistry will be performed to assess structural and cellular changes, e.g., osseous cells, chondrocyte and tenocyte activity, collagen organization, cellular composition, and extracellular matrix changes in the enthesis, bone, and MTJ.
P4
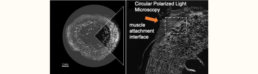
High-resolution imaging and analytics of mineralized bone tissue and soft tissues at the bone-tendon-muscle interfaces
Main Supervisor: Björn Busse (UKE)
Co-Supervisors: Imke Greving (Hereon) & Benjamin Ondruschka (UKE)
Research background and question
Mechanical loading is known to influence the nano- and microstructural properties of the enthesis and MTJ, but how these interfaces adapt to different physiological states remains unclear. Moreover, the ultrastructural characteristics of mineralized tendon-bone interfaces in humans remain poorly understood [1]. The spatial arrangement of mineralized and non-mineralized tissue, collagen fiber orientation, and the relationship between mineral composition and mechanical stability require further investigation. Structural adaptations in physically active individuals may exhibit reinforced mineralization patterns and collagen organization, while immobilized and aging individuals may show reduced mineralization and impaired tendon-bone integration and degenerative changes contributing to joint instability and fracture susceptibility. However, quantitative data on these adaptations, particularly in human tissue samples, remain limited.
Specific aims
- Characterize the 2D/3D ultrastructure of mineralized and non-mineralized tissues at the enthesis and myotendinous junction to identify structural markers linked to interface integrity.
- Investigate microarchitectural differences across distinct physiological states, comparing immobilized individuals, physically active individuals, and elderly populations to understand how mechanical loading and aging influence enthesis adaptation and degeneration.
Work program and methods
This project aims to characterize the ultrastructural features of the mineralized bone-tendon interface across different physiological states using high-resolution imaging across high-risk cohorts (immobilized individuals with prolonged unloading due to spinal cord injury, physically active individuals exposed to high mechanical loading, and elderly individuals experiencing age-related degenerative changes). Circular Polarized light microscopy (CPL), synchrotron micro- and nanoCT, quantitative backscattered electron imaging (qBEI), and focused ion beam scanning electron microscopy (FIB-SEM) will be used to analyze the 2D/3D-dimensional ultrastructural organization at tendon interfaces. A correlative imaging approach will be employed to characterize the ultrastructure and mineral composition of the enthesis. The same suite of imaging and microscopy methods will then be used to analyze the 2D/3D-dimensional ultrastructural organization of fibrous tissues and mineralization patterns at hard-soft and soft-soft interfaces of tendons.
P5
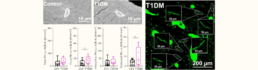
Intra-bone-tissue-interfaces connecting around the osteocyte network: Investigating the relationship between the osteocyte and vascular networks
Main Supervisor: Katharina Jähn-Rickert (UKE)
Co-Supervisors: Maike Frye (UKE) & Tobias Knopp (UKE/TUHH)
Research background and question
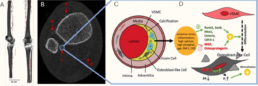
Osteocytes are highly secretory, mechanosensitive cells orchestrate various other cell types with their extensive dendritic network within the bone matrix [1]. Osteocytes directly interact with the vasculature in bone i.e., the intra-cortical vessels, to allow for communication and an exchange of secretory molecules. The structure-function relationship of the network-forming osteocytes implies that a vital network is required to orchestrate physiological reactions. The same is true for the vasculature network, consisting of both blood and lymph vessels [2]. Osteocyte network disruptions are complex and progressive and may include loss of dendritic and, or canalicular connections [3], loss of viable osteocytes, empty lacunae, up to micropetrosis of osteocyte lacunae, as seen in diabetic bone disease (Figure Above) [4]. Similarly, blood perfusion and bone vasculature density are lowered with osteoporosis, osteoarthritis and other bone diseases, which are also characterized with an osteocyte network phenotype, suggesting that both 3D networks are intricately linked.
Specific aims
- Assess pathological changes and identify structure-function alterations in osteocyte and vascular networks using dual-imaging approaches and AI-driven image processing.
- Determine structural mechanisms and processes involved in osteocyte and vascular network replenishment under pathological conditions.
Work program and methods
This project will employ dual-imaging approaches and AI-driven image analysis to examine pathological changes in the osteocyte and vascular networks simultaneously. The first phase will focus on high-resolution imaging of human bone specimens from individuals with diabetic bone disease and microvascular pathology, as well as age-related bone loss with arteriosclerosis. Micro-CT, electron microscopy, and confocal laser microscopy will be used to visualize and quantify both networks within bone matrix. In the second phase, the study will investigate osteocyte and vascular network replenishment mechanisms in different pathological contexts. Surgical bone specimens from knee arthroplasty patients with osteophyte-specific local bone formation will be analyzed to assess localized network regeneration. Additionally, human bone metastasis biopsies with osteosclerotic lesions will provide insight into network remodeling in tumor-affected bone environments.
P6
The impact of the bone microenvironment on endothelial cell behavior and the reciprocal effects of vascular dysfunction on bone quality

Main Supervisor: Maike Frye (UKE)
Co-Supervisors: Imke Fiedler (UKE) & Björn Busse (UKE)
Research background and question
Endothelial cells (ECs) comprise the inner layer of the blood and lymphatic vasculature. While blood vasculature has been proven crucial for bone health, the presence of lymphatic vessels in bone remains controversial, with a recent study reporting functional lymphatics in healthy and regenerating bone [1], while others suggest they only appear under pathological conditions [2]. Unlike other organs, the bone microenvironment is highly stiff, creating a unique environment for ECs [3]. While we have studied how matrix stiffness influences EC function in soft tissues [4], the influence of the bone microenvironment on bone EC behavior, as well as the reciprocal effects of vascular dysfunction and vascular stiffening on bone quality, remain to be investigated.
Specific aims
- Investigate the impact of bone matrix stiffness on endothelial cell behavior, focusing on mechanosensitive pathways in blood and lymphatic vessels.
- Determine how vascular dysfunction affects bone quality, exploring mechanisms that contribute to skeletal fragility and potential strategies for reversing these effects.
Work program and methods
This project entails ex vivo bone tissue analysis, advanced co-culture models, and in vivo disease modeling to examine the interaction between endothelial cells and the bone microenvironment. The first phase will focus on bone and endothelial-proximal stiffness mapping, using mouse and human bone samples to assess the mechanical properties of the vascular-bone interface. Co-culture models of ECs and bone cells will be developed within hydrogels engineered to mimic physiological and pathological bone stiffness, allowing for the controlled study of mechanosensitive endothelial responses. Next, the project will investigate the reciprocal effects of vascular dysfunction on bone quality using zebrafish and mouse models with altered bone stiffness and vascular pathologies. The zebrafish models will leverage newly developed genetic and dietary interventions (P9) to induce changes in bone stiffness and vascular integrity, providing a unique platform for live imaging of vascular remodeling and bone adaptation. Mouse models of vascular disease and endothelial dysfunction will further be used to assess long-term effects on bone health. This project will provide new insights into the role of ECs in bone health, vascular contributions to bone fragility, and potential therapeutic strategies for restoring skeletal-vascular integrity.
P7
Development of spatiotemporal deep learning methods for shear-wave elastographic imaging at soft tissue interfaces

Main Supervisor: Alexander Schlaefer (TUHH)
Co-Supervisors: Sara Checa (TUHH) & Benjamin Ondruschka (UKE)
Research background and question
Elastographic imaging estimates the elastic tissue properties and can be realized with different clinical image modalities, including optical coherence tomography (OCT) and ultrasound (US). Shear wave elastographic imaging (SWEI) is an approach relating shear wave propagation to tissue elasticity, which allows for quantitative estimates. However, variance and deviations in the estimates typically increase for small fields of view [1] and at tissue interfaces, where wave propagation is complex due to reflection and refraction. Moreover, assumptions like isotropic tissue behavior and in-compressibility are often not fulfilled in real soft tissue [2]. Machine learning (ML) approaches help overcoming these issues [3,4]. However, high-resolution volumetric elastography of musculo-skeletal tissue at interfaces, in different load states, and for larger regions is still largely unexplored. Extending ML methods has the potential to improve analysis of soft-tissue interfaces, e.g., bone-tendon, tendon-muscle or tendon-tendon, and to compare soft tissue properties to obtain information on tissue health.
Specific aims
- Establish suitable imaging parameters and machine learning architectures to estimate elastic tissue properties at interfaces in 2D, 3D and 4D from raw signals and with high resolution.
- Consider shear wave propagation at tissue interfaces and study end-to-end deep learning for detection and compensation of interface related artifacts.
Work program and methods
The project will focus on extending work on Deep Learning (DL) methods for motion tracking [5] and elastography [6] to volumetric elastography of musculoskeletal tissue, see Figure above. Using fully configurable research US and OCT devices we will setup fast volumetric imaging with a small field of view. A robotic lab setup will be adapted to obtain large amounts of data from phantoms and ex-vivo tissue samples with interfaces. We will study recent DL approaches to estimate elasticity in small regions, to obtain high-resolution estimates of larger structures like tendons and muscle by motion tracking and volume stitching, and whether artifacts at interfaces can be mitigated by high-resolution and spatio-temporal DL models. The methods will be evaluated on musculoskeletal tissue interfaces.
P8
Assessing the mechanical damping effect of fat in vertebral bone

Main Supervisor: Alexander Düster (TUHH)
Co-Supervisors: Björn Busse (UKE) & Imke Fiedler (UKE)
Research background and question
Besides its general impact on bone biomechanics and fracture risk, marrow fat can impact the damping properties of bones, which may contribute to bone remodeling and the development of osteoporosis [1-3]. Developing a detailed computational model based on CT scans could provide valuable insights into how marrow fat affects the mechanical properties of vertebral bone. A central method of our research is the Finite Cell Method (FCM), which is highly suitable for this project due to its ability to simulate microstructured/heterogeneous materials derived from CT scans [4,5]. This method has been effectively employed in CT-based structural analyses of bones, as demonstrated in the work by Schillinger et al. [6], see Figure above. This project aims to investigate the influence of fat in vertebral bone by employing and advancing the Finite Cell Method and Spectral Cell Method to simulate the bone’s elastodynamic behavior, elucidating a potential risk factor for fractures and metabolic bone disease.
Specific aims
- Develop a computational model based on CT scans and the FCM to study the influence of fat on the mechanical damping behavior of vertebral bone.
Work program and methods
CT scans from vertebral bones will be used as a starting point for a dynamical simulation based on the FCM. Using CT data, a spatial discretization will be derived to form the foundation of the analysis. The study will explore various modeling approaches, each with different levels of complexity, to accurately represent the presence of fat within the bone. Dynamic simulations in the time domain, which include varying volume fractions of fat, will be used to examine and understand the bone’s damping properties. This numerical model will enable us to assess whether bone remodeling can take place in order to maintain optimal damping, which may be compromised by increased fat content. Ultimately, the project will seek to determine whether such remodeling is associated with the development of osteoporosis, resulting from increased marrow fat content.
P9
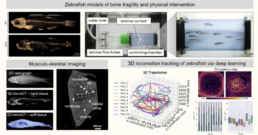
Assessing musculoskeletal intervention using zebrafish locomotion analyses and tissue phenotyping
Main Supervisor: Imke Fiedler (UKE)
Co-Supervisors: Alexander Schlaefer (TUHH) & Maike Frye (UKE)
Research background and question
Zebrafish provide a valuable preclinical model for investigating MSK function and tissue interfaces due to large evolutionary conservation of bone, muscle, and vascular pathways [1-4]. Their small size, ease of genetic manipulation, and capacity for in vivo drug administration enable high-throughput studies of locomotion and tissue-specific phenotyping. However, comprehensive MSK phenotyping combined with deep-learning-based locomotion tracking remains a largely unexplored approach in zebrafish research [5]. Performing correlative functional analyses of the MSK system in zebrafish models of disease can help to better understand osteosarcopenic-vascular mechanisms and assess the effects of interventive measures on locomotion patterns and physical capacities. Recent work within the ICCIR has brought forward a deep-learning based imaging pipeline for efficient tracking of 3D locomotion patterns of zebrafish based on deep learning (Figure above). This zebrafish locomotion tracking pipeline has been already developed for wild type zebrafis and correlate zebrafish MSK tissue phenotypes with locomotion patterns, musculoskeletal activity, and swimming performance.
Specific aims
- Establish zebrafish models with conditions impairing the MSK system for intelligent motion tracking and testing effects of exercise- and treatment-based intervention measures.
- Correlate MSK tissue phenotypes of zebrafish models with locomotion patterns, musculoskeletal activity, and swimming performance.
Work program and methods
Zebrafish models of sarcopenia, bone defects and vascular disease will be used and combined to create new models of multifactorial MSK conditions. Physical exercise protocols as well as medical intervention protocols will be applied with the aim to regenerate musculoskeletal health. Disease models will be subjected deep-learning based 3D locomotion tracking to monitor physical performance and to extract disease patterns, and will undergo multi-scale ex vivo characterization of their hard and soft tissues and interfaces (e.g., bone, muscle, fat, tendons, vessels) based on multimodal imaging from the whole body (microCT) to the nanoscale (e.g., Raman imaging and spectroscopy, confocal imaging, synchrotron nanoCT, and volume electron microscopy [6]).
P10
What are the sex-specific vascular-driven mechanisms contributing to changes in gait and motion?
Main Supervisor: Felix v. Brackel (UKE)
Co-Supervisors: Alexander Schlaefer (TUHH) & Maike Frye (UKE)
Research background and question
In conditions such as peripheral artery disease, reduced perfusion leads to muscle fatigue, altered gait patterns, and impaired movement coordination, often resulting in fall risk and mobility decline. However, the extent to which arterial calcification, vascular remodeling, and sex-specific factors influence gait and motion biomechanics has yet to be fully understood. Despite growing interest in bone-muscle-vascular interactions, most studies have not systematically examined the impact of vascular health on gait and motion, nor have they adequately integrated sex-specific analyses. Existing studies primarily focus on bone and muscle composition but fail to capture functional movement patterns and vascular dynamics. In a previous pilot study of 300 patients at UKE, we analyzed the relationship between bone structure and lower-limb vascular calcifications, identifying sex-specific differences in bone remodeling and vascular changes [1]. However, this study lacked functional neuromuscular assessments, such as gait analysis, movement efficiency, and postural stability. To address this gap, a large-scale, data-driven study is needed, integrating vascular imaging, neuromuscular performance assessments, and computational modeling to uncover the sex-specific, vascular-driven mechanisms shaping movement patterns.
Specific aims
- Define sex-specific vascular-driven gait alterations in patient data.
- Identify patterns that may predict functional decline and fall risk und neuromuscular disease.
Work program and methods
A comprehensive dataset will be assembled with retrospective analysis of HR-pQCT, DXA and neuromuscular test data available in existing clinical datasets. Neuromuscular data includes gait and balance metrics from Romberg balance tests, and sit-to-stand motion tracking from chair-rising tests, including power and speed data. Computational workflows will be established for automated segmenting calcified arteries, muscle tissue, and bone, enabling quantitative vascular assessments. Subsequently, a neural network-based movement analysis will assess postural stability and dynamic gait changes in relation to vascular health, obtaining a predictive model of gait alterations based on vascular and neuromuscular data.